On August 4, 2021, the Centers for Medicare and Medicaid Services (CMS) published the final rule for the fiscal year (FY) 2022 Inpatient Psychiatric Facilities Prospective Payment System (IPF PPS), which impacts freestanding psychiatric hospitals and excluded psychiatric units.
The regulations become effective October 1, 2021. An overview of the final rule follows.
Final Changes to IPF Payments
CMS finalized the following updates to the prospective payment rates, outlier threshold, and wage index for the IPF PPS.
IPF PPS Rates
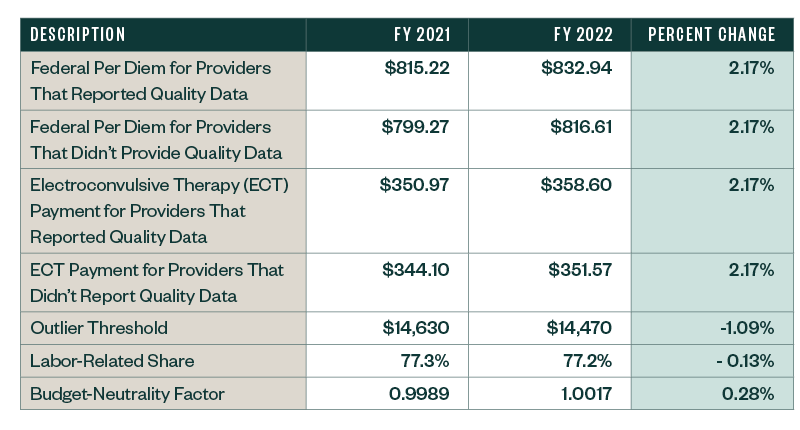
Other Notable Updates
Core-Based Statistical Area (CBSA) Designation
CMS chose not to adopt Bulletin No. 20-01 for FY 2022 because it didn’t materially impact the Inpatient Psych Wage Index data.
Inpatient Psychiatric Facilities Quality Reporting
According to the final rule, CMS will make the following changes to the Inpatient Psychiatric Facilities Quality Reporting (IPFQR) program:
- Adopt voluntary patient-level data reporting for chart-abstracted measures for data submitted for the FY 2023 payment determination and mandatory patient-level data reporting for chart-abstracted measures for the FY 2024 payment determination and subsequent years
- Revise CMS regulations at 42 CFR 412.434(b)(3) by replacing the term QualityNet system administrator with QualityNet security official
- Adopt the Coronavirus Disease 2019 (COVID-19) Vaccination Coverage Among Health Care Personnel (HCP) measure for the FY 2023 payment determination and subsequent years
- Adopt the Follow-up After Psychiatric Hospitalization (FAPH) measure for the FY 2024 payment determination and subsequent years
CMS removed the following measures for FY 2024 payment determination and subsequent years:
- Timely Transmission of Transition Record (Discharges from an Inpatient Facility to Home/Self Care or Any Other Site of Care) measure
- Follow-up After Hospitalization for Mental Illness (FUH) measure
CMS won’t finalize proposed rules to remove the following measures for FY 2024 payment determination and subsequent years:
- Alcohol Use Brief Intervention Provided or Offered and Alcohol Use Brief Intervention Provided measure
- Tobacco Use Treatment Provided or Offered and Tobacco Use Treatment measure
Economic Impact
The overall economic impact of the final FY 2022 changes equates to an $80 million increase in payments from FY 2021.
Next Steps
Providers need to review whether the appropriate IPF rates have been loaded into their patient accounting system used to bill Medicare on or after October 1, 2021.
Once these revised rates are incorporated, it’s important to validate that the rates are calculating appropriately.
This can be accomplished by pulling a paid claim and running it through the IPF pricer tool that can be downloaded from the CMS website.
We’re Here to Help
For more information about the final rule, the revised rates, or assistance during your validation review, contact your Moss Adams professional.