On August 4, 2021, the Centers for Medicare & Medicaid Services (CMS) published the final rule for fiscal year (FY) 2022 Inpatient Rehabilitation Facility Prospective Payment System (IRF PPS) in the Federal Register. The regulations take effect October 1, 2021.
Each year, CMS publishes updates to the regulations for inflation factors, wage adjustments, and other patient-care payment adjustments. An overview of the FY 2022 IRF PPS, including finalized changes and other relevant updates, follows below.
Finalized Changes to IRF Payments
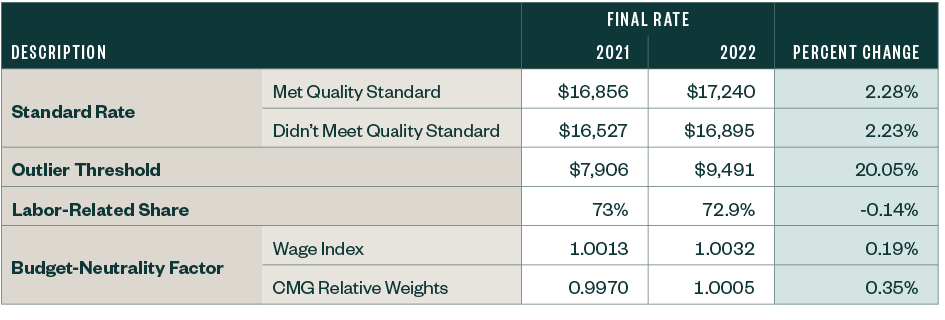
Other Notable Updates
Core-Based Statistical Area Designation
The FY 2022 IRF PPS final rule doesn’t adopt the most recent Office of Management and Budget (OMB) Core-Based Statistical Area (CBSA) delineations and applies a five-percent cap on any wage index decrease.
Coverage Requirements
The final FY 2022 IRF PPS rule includes updates to coverage requirements. Some of these requirements include updates to COVID-10 policies and procedures.
Additional Updates
Other provisions of the final rule include updates as proposed to the following:
- Case mix group (CMG) relative weights and average length of stay values for FY 2022, in a budget-neutral manner
- IRF PPS payment rates for FY 2022 by the final market-basket increase factor—based on the most current data available—with a final productivity adjustment required by Section 1886(j)(3)(C)(ii)(I) of the Social Security Act
- Descriptions of the calculation of the IRF standard payment conversion factor for FY 2022
- Cost-to-charge ratio (CCR) ceiling and urban and rural average CCRs
- Descriptions of the method for applying the reduction to the FY 2022 IRF increase factor for IRFs that fail to meet the quality reporting requirements
Economic Impact
The overall economic impact of this rule is an estimated $130 million in increased payments from the US federal government to IRFs during FY 2022.
Next Steps
Providers need to review whether they’ve loaded the appropriate IRF rates into the patient accounting system they use to bill Medicare on or after October 1, 2021.
Once they incorporate these revised rates, they can follow best practices and validate that the rates calculate appropriately.
The provider can accomplish this by pulling a paid claim and running it through the IRF pricer downloadable from the CMS website.
We’re Here to Help
For more information about the rule and its implications or assistance during your validation review, contact your Moss Adams professional.