On August 1, 2022, the Centers for Medicare & Medicaid Services (CMS) published the final rule for fiscal year (FY) 2023 Inpatient Rehabilitation Facility Prospective Payment System (IRF PPS) in the Federal Register. The regulations will take effect October 1, 2022.
Each year, CMS publishes updates to the payment rates and regulations for inflation factors, wage adjustments, and other patient-care payment adjustments. An overview of the FY 2023 IRF PPS, including finalized changes and other relevant updates, follows below.
Finalized Changes to 2023 IRF Payments
CMS finalized the following updates to inpatient rehabilitation facility (IRF) rates.
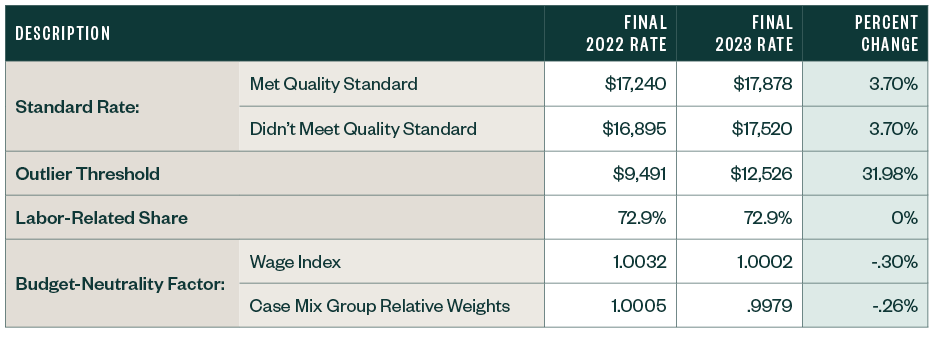
Other Notable Updates
Core-Based Statistical Area Designation
The FY 2023 IRF PPS final rule doesn’t adopt the most recent Office of Management and Budget (OMB) Core-Based Statistical Area (CBSA) delineations, as was the case in FY 2022.
Wage Index Cap
CMS finalized permanent rules to its FY 2021 temporary policy of limiting year-over-year wage index decreases to 5%.
As such, the FY 2023 wage index won’t be less than 95% of its final wage index for FY 2022. For subsequent years, a provider’s wage index won’t be less than 95% of its prior year wage index.
IRF Teaching Policy
CMS finalized codification of its existing teaching status adjustment policy through final amendments to the regulation text and also finalized updates and clarification to the IRF teaching policy with respect to IRF hospital closures and displaced residents.
Facility Level Adjustment Factors
In the proposed rule, CMS solicited comments on the methodology used to determine the facility-level adjustment factors including:
- Rural adjustment factor
- Low-income patient adjustment factor
- Teaching status adjustment factor
In the final rule, CMS didn’t address specific comments related to the above but did state they would take all comments into consideration for future development of payment policies.
IRF Transfer Policy
The Office of Inspector General’s recommendation resulted in a proposed rule that solicited comments regarding the expansion of the IRF transfer payment policy to apply to discharges to home health.
In the final rule, CMS also didn’t address specific comments related to the above but did state they would take all comments into consideration for future development of payment policies.
IRF Quality Reporting Program (QRP)
The rule finalizes requirements to quality data reporting on all IRF patients beginning with the FY 2026 IRF QRP and amends regulations to be consistent with the final requirements. This rule also corrects an error in the regulations text at Section 412.614(d)(2).
Additionally, CMS requested comments on three issues in its proposed rule:
- Future measure concepts under consideration for the IRF QRP
- Future digital quality measure for the IRF QRP
- Overarching principles for measuring equity and health quality disparities across CMS quality programs, including the IRF QRP
In the final rule, CMS did not address specific comments related to the above but did state they would take all comments into consideration for future development of payment policies.
Economic Impact
The overall economic impact of this rule is an estimated $275 million in increased payments from the US federal government to IRFs during FY 2023.
Next Steps
Providers need to review whether they’ve loaded the appropriate IRF rates into the patient accounting system they use to bill Medicare on or after October 1, 2022.
Once they incorporate these revised rates, they can follow best practices and validate that the rates calculate appropriately.
The provider can accomplish this by pulling a paid claim and running it through the IRF pricer on the CMS website.
We’re Here to Help
For more information about the rule and its implications, contact your Moss Adams professional.
You can also find more insights on our Provider Reimbursement Enterprise Services page.